By Sara Lyle-Ingersoll, Cervivor Communications Director
Happy 20th birthday, HPV vaccine!
Two decades is a big deal. Cervivor marked the same milestone last year, so we know a bit about what 20 years of impact feels like.
We still remember the excitement in 2006 when the first HPV vaccine was approved by the U.S. Food and Drug Administration (FDA). The news made the cover of Time magazine and the front page of The New York Times. But it wasn’t just another medical headline — it was a major scientific breakthrough. The idea that we could prevent cervical cancer before it ever started felt revolutionary. The hope was palpable.
Which makes today, International HPV Awareness Day — part of the International Papillomavirus Society‘s (IPVS) annual campaign to promote HPV prevention, screening, and care — a fitting moment to say happy birthday, thank you, and keep up the good work. Consider this our love letter to you, HPV vaccine.
Why We Love You
Let’s start with the obvious: You prevent cancer.
Not symptoms. Not severity. Cancer.
HPV is incredibly common — about 80% of people will be infected at some point in their lives. Most infections clear on their own, but some persist and can lead to cancer. Globally, HPV causes nearly all cervical cancers and contributes to cancers of the anus, oropharynx (throat), vulva, vagina, and penis. Together, HPV-related cancers account for more than 720,000 new cancer cases and roughly 350,000 deaths worldwide each year.
When you were first approved in 2006, you protected against four HPV types, including types 16 and 18, which cause the majority of cervical cancers. Today’s version protects against nine HPV types: seven responsible for about 90% of cervical cancers, plus two that cause most genital warts. That’s pretty badass. Pardon our language.
Because prevention works best before infection occurs, vaccination is recommended between age 11 and 12, and can be given as early as 9. In this video for HPV Day 2026, IPVS envisions a world free from the cancer-causing virus — made possible in large part by you.
Your Track Record Speaks for Itself
More than half a billion doses of the HPV vaccine have been given out worldwide, and decades of safety monitoring across multiple countries continue to confirm that you are safe.
Any side effects are typically mild and temporary, and serious reactions are rare. The Centers for Disease Control and Prevention (CDC), the World Health Organization (WHO), and numerous independent reviews consistently affirm your safety.
And are you effective? Heck, yes! The data is just as strong.
Countries with high vaccination coverage — think Australia, Rwanda, Sweden — have documented dramatic declines in HPV infections, genital warts, and high-grade cervical precancers among young people.
This is no longer about projections or promises. The receipts are in. Here are just a few:
- A landmark 2020 study published in The New England Journal of Medicine found that Swedish girls vaccinated before age 17 had an 88% lower risk of cervical cancer compared to unvaccinated peers.
- In the U.K., research published in The Lancet in 2021 showed nearly a 90% reduction in cervical cancer among women vaccinated between 12 and 13.
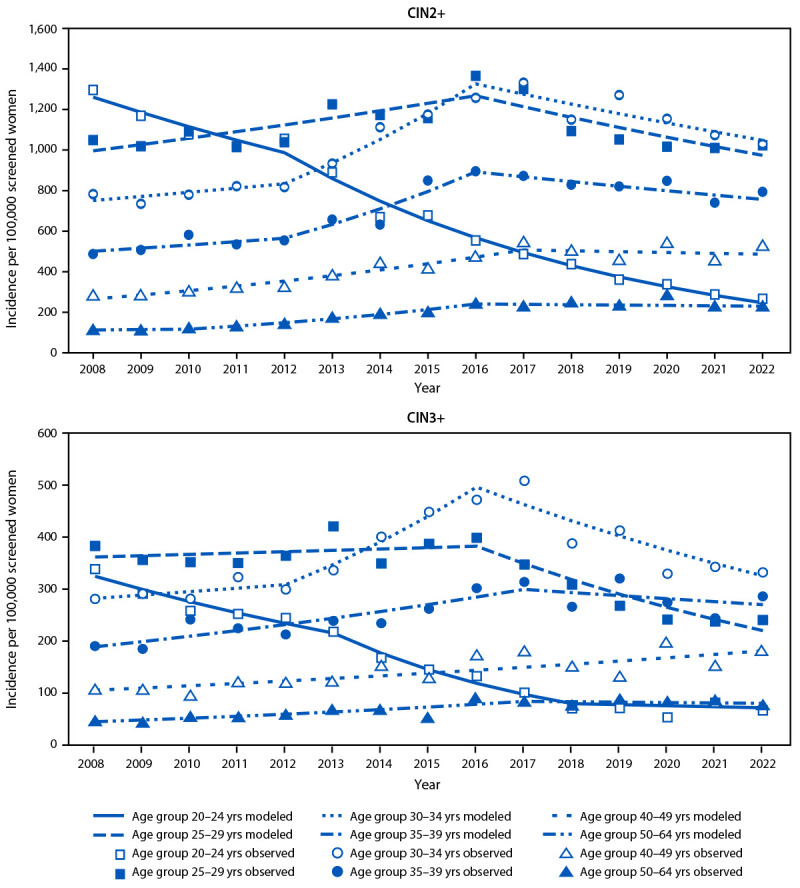
- In the U.S., a 2025 CDC analysis of 2008–2022 data found that cervical precancers among women 20 to 24 — the first generation routinely vaccinated — declined by roughly 80%.
That’s measurable progress and lives saved. Wow, just wow.
We Know It Hasn’t Always Been Easy
From the beginning, you carried more than a syringe and a schedule. You carried stigma — something anyone affected by a below-the-belt cancer understands all too well.
Because HPV is transmitted through intimate contact, conversations about the vaccine have often been wrapped up in discomfort, misinformation, and politics. Some struggle discussing a sexually transmitted virus with preteens. Others falsely claim you’re a “permission slip” for promiscuity.
At the recent 2026 Cervical Cancer Summit — while unpacking your complicated history — Chief Medical Officer of the Association of Immunization Managers Michelle Fiscus, MD, FAAP, shared an old cartoon poking fun at the promiscuity myth. It showed a young girl receiving the HPV vaccine and saying, “I am so turned on right now.” The joke landed because the premise was so absurd.
A vaccine does not change a child’s values or lifestyle choices. It reduces their risk of cancer. Full stop.

In Case You Need to Hear This
Progress hasn’t been perfect — but that’s not on you.
Vaccination rates vary widely by region and community. In the U.S., HPV vaccination coverage among adolescents continues to improve, but it still trails other routine adolescent vaccines like Tdap and meningococcal, according to the CDC. Research shows that a strong provider recommendation is one of the biggest factors in increasing HPV vaccination.
Globally, cervical cancer disproportionately affects women in low- and middle-income countries, where access to both vaccination and screening can be limited. The WHO’s strategy to eliminate the disease as a public health problem calls for 90% of girls to be fully vaccinated against HPV by age 15.
It’s simple math: The more people who receive you, the more lives will be saved from HPV-related cancers — which is why we’re your hype girl today and every day.

Keep On Keeping On!
HPV vaccine, you have given us a tool that previous generations couldn’t even dream of.
Twenty years ago, approving the first HPV vaccine was an act of scientific courage and public health ambition. Today, the challenge is simpler — and harder. We have to use it.
Reflecting on the momentum of the first National HPV Conference last April, Cervivor Founder and Chief Visionary Tamika Felder said, “Knowledge is power, but this is just the start. Preventable cancers like cervical cancer are on the rise because of complacency, stigma, and misinformation. The time to prevent suffering — and save lives from cervical and other HPV-related cancers — is now.”
Your moment is now.
Happy 20th birthday to a vaccine that prevents cancer.
Here’s to a future when a cervical cancer diagnosis or, worse, a death is ancient history.
P.S. Congratulations to the St. Jude HPV Cancer Prevention Program on five years of saving lives by increasing HPV vaccination rates! We couldn’t be prouder to call you a partner.
About the Author

SARA LYLE-INGERSOLL is a content and communications expert dedicated to transforming lived experiences into impactful stories. Her award-winning magazine feature about a close friend who passed from cervical cancer in their twenties led her to connect with Cervivor’s founder, Tamika Felder, and solidified her commitment to cervical cancer awareness and prevention. Now, as Cervivor’s Communications Director, Sara brings this mission full circle.